Hello!Thank you for sharing valuable information about ivf clinic. I hope you will share some more information about infertility treatment. please keep sharing! we are very grateful to you.

Infertility can be a scary journey.
There are so many unknowns and so many things beyond your control.
Never mind the million and one questions swimming through your head at any time…
How long is it actually supposed to take?
Should I see a fertility specialist?
How much will fertility treatments cost?
Is it better to try intrauterine insemination (IUI) or go straight to IVF?
How many injections will I have to do?
… and the list of unnerving questions goes on.
Instead of getting discouraged or succumbing to the sheer overwhelm of it all, we are here to arm you with some important facts and statistics about infertility.
And even if you aren’t starting a family just yet, it could still benefit you to get acquainted with some of this important information to better prepare yourself for the future. Plus, you might learn something that could support a friend or family member struggling with infertility.
Here’s a quick overview of what you’ll discover:
Watch the Video Recap:
How is Infertility Defined?
Infertility is typically defined as the inability to conceive after one year of having regular, unprotected sex if the female partner is < 35 years of age, or after 6 months if ≥ 35 years of age.
Fast Facts When Trying to Get Pregnant
-
You and your partner have the highest chance of conceiving in the first 3 – 6 months of trying to get pregnant.
-
For young couples in good health, the chance of conception is between 20 – 37% during the first 3 months. The chance of success increases to 85% by one year (the majority of which will conceive within the first 6 months of trying) and 95% after two years of trying.
-
The highest likelihood of conceiving in any given cycle is 15-20% which is actually much lower than most people think!
And just in case you’re curious, cycle fecundability is the probability that a menstrual cycle will result in a pregnancy. On the other hand, fecundity is the probability that a cycle will result in live birth. The concept of fecundability and fecundity sounds a little strange at first which is why we thought you might like to know.
Who Struggles With Infertility?
Anyone can struggle with fertility problems, regardless of age, gender, ethnicity, race, or sexual orientation.
According to the Centers for Disease Control and Prevention (CDC), roughly 10% of women under the age of 44 have trouble conceiving or staying pregnant. In other words, 6.7 million couples in the United States face some difficulty when trying to conceive. And when we look at data from across the world, about 48.5 million couples experience infertility.
Now we probably don’t have to remind our female followers, but it’s incredibly important to remember that infertility affects men about as often as it affects women. In fact, one-third of fertility issues are due to the man (i.e., male factor infertility)!
So, as most fertility specialists will tell you…
-

⅓ of infertility cases are due to ovulatory dysfunction
-

⅓ of infertility cases are due to decreased sperm counts
-

⅓ of infertility cases are completely unknown (unexplained infertility)
Beyond this, the majority of the remaining causes of infertility are due to factors that impact fallopian tube function or endometriosis.
Regardless of which party is struggling with reproductive problems, know that you are not alone. Several sources show that 1 out of every 8 couples trying to conceive experience some infertility issues along the way.
What Causes Fertility Issues?
Pregnancy is nothing short of a miracle.
Several well-coordinated steps of our reproductive systems must successfully occur for you and your partner to get pregnant.
To quickly review, here are the events that must happen in perfect sequence:
-

A woman’s body must release an egg from one of her ovaries (i.e., ovulation).
-

A man’s sperm must join with the egg along the way (i.e., fertilization).
-

The fertilized egg (embryo) must pass through the fallopian tube.*
-

The embryo must attach to the inside of the uterus (i.e., implantation).
* It’s a subtle point, but one worth highlighting… fertilization happens in the fallopian tube NOT the uterus – pretty cool, right?
As you can imagine, a problem with any one of these steps (or even more than one) can lead to infertility. And without getting too far in the weeds, let’s take a closer look at the common causes of male infertility and female infertility.
Common Male Fertility Issues
“Male factor” plays a role in up to 50% of the time with infertility. It’s the primary contributing factor about ⅓ of the time, but it seems to get much less attention compared to female-related factors.
The initial evaluation of the male partner – beyond a detailed history and physical – involves a semen analysis. A semen analysis assesses a variety of factors including sample volume as well as sperm concentration, sperm motility, and sperm morphology.
Common contributing factors to male infertility include things like certain medicines (e.g., testosterone supplementation), varicocele (i.e., dilated veins surrounding the testicles), and idiopathic (i.e., unexplained).
Genetic factors and lifestyle factors like smoking can contribute to decreased sperm production and male infertility as well.
If your physician notes decreased sperm parameters in your male partner, most commonly he’ll be referred to a urologist who specializes in male fertility for a more detailed exam and laboratory evaluation. We know it goes without saying, but it’s just as important for men to get a complete evaluation and address important lifestyle factors like diet, exercise, alcohol, and tobacco use.
Common Female Fertility Issues
One of the most common female infertility factors is ovulatory dysfunction, which results in menstrual cycle irregularity. This can happen for a variety of reasons, including abnormal signaling from your pituitary gland in the brain. Women with polycystic ovary syndrome (PCOS) commonly experience issues with ovulatory dysfunction.
Other issues affecting female fertility include fibroids and endometriosis, which can result in distorted pelvic anatomy as well as increased inflammation. Tubal factor (where something is blocking the fallopian tube so the sperm and egg can’t meet), and decreased ovarian reserve (decreased egg number) are also common contributors.
Unexplained infertility (where everything checks out normal and the doctors can’t tell you what might be contributing) typically makes up the remaining causes of infertility.
As you can see, infertility can be caused by any number of medical problems. If you think you may be dealing with a fertility issue, it’s important to see a fertility specialist to discuss your situation and discover your treatment options.
Important Fertility Statistics and Data
There are many different statistics and numbers to consider when facing infertility. Some of the more important things to consider include egg count, the chance of pregnancy with and without assisted reproductive treatments (ART), and the risk for genetic disease.
Egg Count Over Time
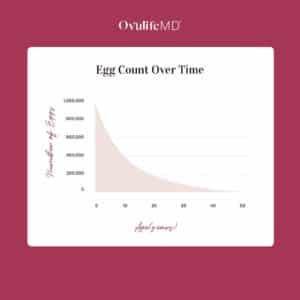
A woman is born with all the eggs she’ll ever have, which at birth, is typically around 1-2 million. Unlike men who are always producing new sperm to replenish their sperm count, females stop making eggs.
Surprisingly enough, even though a female doesn’t typically start menstruation until she is between the ages of 10-14, eggs are constantly being lost throughout infancy and adolescence. In fact, by the time a woman reaches puberty, she only has 300,000-400,000 eggs left in her ovaries.
Starting around the age of 37, egg count starts to rapidly decline and by the time a woman hits 40, the number of eggs remaining is somewhere between 5,000 – 10,000.
Chance of Natural Pregnancy by Age
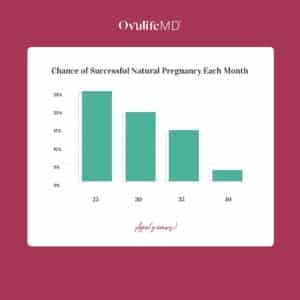
Women under the age of 35 have approximately a 15-20% chance of getting pregnant naturally each cycle. By the age of 40, the chance of getting pregnant naturally each month is only about 2-5%.
Chance of Pregnancy for Patients Using IVF
Assisted reproductive technology (ART), including in-vitro fertilization (IVF), may be recommended when other techniques for getting pregnant have not been successful.
But before you start IVF, it’s important to note that this procedure does not give you a 100 percent chance for a healthy pregnancy. Ultimately, IVF success varies with many factors, age being the most important if you use your own eggs.
Here’s a quick breakdown of the numbers based on nationwide data from 2019:
-

For women < 35 years old, live birth per cycle is ~ 50%
-

For women 35 – 37 years old, live birth per cycle is ~30%
-

For women 38 – 40 years old, live birth per cycle is ~20%
-

For women 41 – 42 years old, live birth per cycle is ~10%
-

For women 43 – 44 years old, live birth per cycle is ~3%
The Society for Assisted Reproductive Technologies (SART) tracks IVF success rates nationwide on their website. They also break down the numbers by diagnosis, age, cycle type and you can even look at your individual clinic success rates. This can be incredibly helpful for infertile couples when choosing the best practice on their journey. Another resource for this information is the CDC’s website.
Risk of Abnormal Pregnancy
For women who achieve pregnancy, the chance of a genetic abnormality increases with age. As you can see below, the risk increases significantly between the ages of 35 and 40.
Genetic abnormalities can result in miscarriage or a baby with medical conditions such as autosomal trisomy’s, including Down Syndrome or an imbalanced number of chromosomes. This is why many fertility specialists will recommend freezing eggs at a younger age sometimes, even if they are used at a later time.
If you’re interested in a helpful egg banking calculator that demonstrates the likelihood of future pregnancy based on the age at which you froze eggs and how many are frozen, then check out this link from MD Cal.
Here’s a quick breakdown of the numbers:
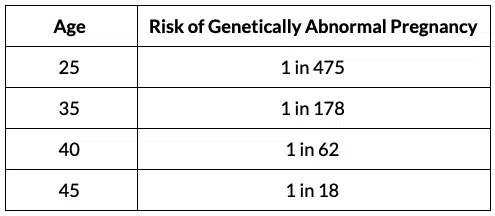
Hopefully, these statistics are starting to answer some of your more burning questions. If you have more questions, simply drop them in the comments below and we’ll do our best to help you find the answers. The websites below also have great frequently asked questions (FAQs) worth checking out:
-

The National Infertility Association (Resolve)
-

The Society for Assisted Reproductive Technology (SART)
-

American Society for Reproductive Medicine (ASRM)
How to Naturally Increase Fertility as a Woman
Depending on your insurance coverage, the average cost of a single IVF cycle in the U.S. is between $10,000 and $15,000… That means you probably want to do everything you can to increase your chances of success before or even during infertility treatment.
Luckily, there are many lifestyle factors that have been scientifically proven to have a tremendous impact on your reproductive health… And when working with our patients we always focus on three key areas:
Overriding fertility threats.
Vitalizing and nourishing the body.
Uniting the mind-body connection.
The OvuMethod is actually our integrative approach to naturally optimizing fertility. Let’s quickly summarize each of these steps so you have a better idea of how to make them work for you!
Overriding fertility threats is all about removing the toxins that are harming our bodies. Whether that be the food we eat or chemicals in our environments, it’s critical to access these threats and take steps to minimize them when possible.
Vitalizing and nourishing the body is focused on fueling our bodies with pro-fertility foods and getting the right amount of exercise. There are many unique aspects to fertility-friendly exercise and nutrition that go beyond “eating clean” and taking 10,000 steps per day.
Uniting the mind-body connection is one of the most important steps on any woman’s fertility journey. It goes without saying that infertility is stressful and self-care is important. Having the ability to center yourself will help you find peace during the storm.
If any aspect of this approach resonates with you, we invite you to download our free Fertility Optimization Guide that shows you exactly how to put this info into action.
Final Thoughts
Before you decide to start a family, make sure you empower yourself with some of the basic facts and statistics about infertility. Fertility struggles are more common than people think, and it’s important to know that you’re not alone in this.
Whenever you’re ready, discover how to naturally optimize your fertility without the confusion and overwhelm and finally take the RIGHT steps to grow your family today!
If you enjoyed this post, get more like it
Always evidence-based. Always actionable.
And just like a good doctor’s visit, your privacy is protected
Don't worry, you can always unsubscribe with just one click.Welcome to the tribe!
You’ve joined the OvulifeMD community. Don’t forget to check your inbox for a special welcome email.
Featured Content

Leave a comment
If you have any questions, we will be happy to answer them.
Thanks for sharing what's on your mind!
Check the thread for more insight and support.




Hello!Thank you for sharing valuable information about ivf clinic. I hope you will share some more information about infertility treatment. please keep sharing! we are very grateful to you.