
After weeks of wondering what has been going on with your body, you leave your doctor’s office with a useless piece of paper entitled, “What You Need to Know About Your PCOS Diagnosis”.
A million questions begin running through your head, none of which can be found on that paper.
You are NOT alone!
And if you haven’t been diagnosed with Polycystic Ovarian Syndrome (PCOS), then chances are you know someone affected by it. In fact, PCOS is one of the most common endocrine disorders affecting approximately 1 in 10 reproductive-age women.
PCOS is a complex condition that impacts your fertility, metabolism, and mental health – all of which often go undiagnosed or unaddressed until women have difficulties trying to conceive.
And given that it’s so complex, there’s a lot of misinformation out there. Unfortunately, this misinformation is partially due to gaps in knowledge among both patients and doctors when it comes to understanding the diagnostic criteria.
Of course, any confusion surrounding PCOS is certainly not helped by the inaccurate and misguided information found on social media and the internet.
So here we are… Hoping to clarify, dispel, and set the record straight over the course of this 4-part blog series in recognition of PCOS awareness month (and every month thereafter).
Part 1: How to diagnose PCOS (and no, “cysts on ovaries” are actually not required).
Part 2: First-line treatment for PCOS – lifestyle modifications (we’ll cover the dietary changes that are actually backed by evidence).
Part 3: What’s the best type of exercise for PCOS?
Part 4: Supplements for PCOS – do they really work?
Let’s jump into Part 1 – How To Diagnose PCOS!
Here’s a quick overview of what you’ll discover:
How To Accurately Diagnose PCOS
PCOS is all about understanding what’s required and what’s NOT required to make the proper diagnosis.
The most common diagnostic criteria for PCOS is the Rotterdam Criteria, which requires 2 out of the 3 following clinical criteria to be met:

Hyperandrogenism
The term hyperandrogenism is just a fancy way of describing when high levels of androgens (hormones that play a role in male reproductive traits and activity) are present in females.
Androgens may be referred to as “male hormones,” but don’t let this fool you. Both men and women produce androgens, just in differing amounts.
The principal androgens in our bodies are testosterone and androstenedione. Other androgens include dihydrotestosterone (DHT) and dehydroepiandrosterone (DHEA). In women, one of the primary purposes of androgens is to be converted into estrogens.
Okay, enough basic science…
Clinical signs of hyperandrogenism can include:
-
Hirsutism – excessive course terminal hair growth in a male-like pattern (upper lip, chin, abdomen, chest, inner thighs, and back). Of note, this does not include the lighter, softer fine (vellus) hair growth that many women experience in these areas.
-
Alopecia– central loss of hair on the head (a symptom that is incredibly bothersome but not as many people know about).
-
Cystic/inflammatory acne – a severe form of acne with painful and infected nodules that are often resistant to medication.
-
Acanthosis nigricans – rough, darkly pigmented areas of skin.
Biochemical signs of hyperandrogenism include elevated blood levels of:
-
Bioavailable testosterone
-
DHEA-S
-
Androstenedione
Note that it’s not recommended that all of these be assessed when making the diagnosis of PCOS (expert recommendation is to assess bioavailable or calculated free testosterone), but are worth noting when discussing biochemical hyperandrogenism.
Polycystic ovaries
It’s important to note that just having polycystic appearing ovaries on ultrasound does NOT mean you have PCOS in the absence of other symptoms.
Yes, you read that correctly – your ovaries can be polycystic appearing but you don’t necessarily have PCOS. On the flip side, your ovaries can look totally normal and you can actually still have PCOS. Remember, it all comes down to having 2 out of the 3 diagnostic criteria.
Before moving on, let’s address what it means to have polycystic appearing ovaries…
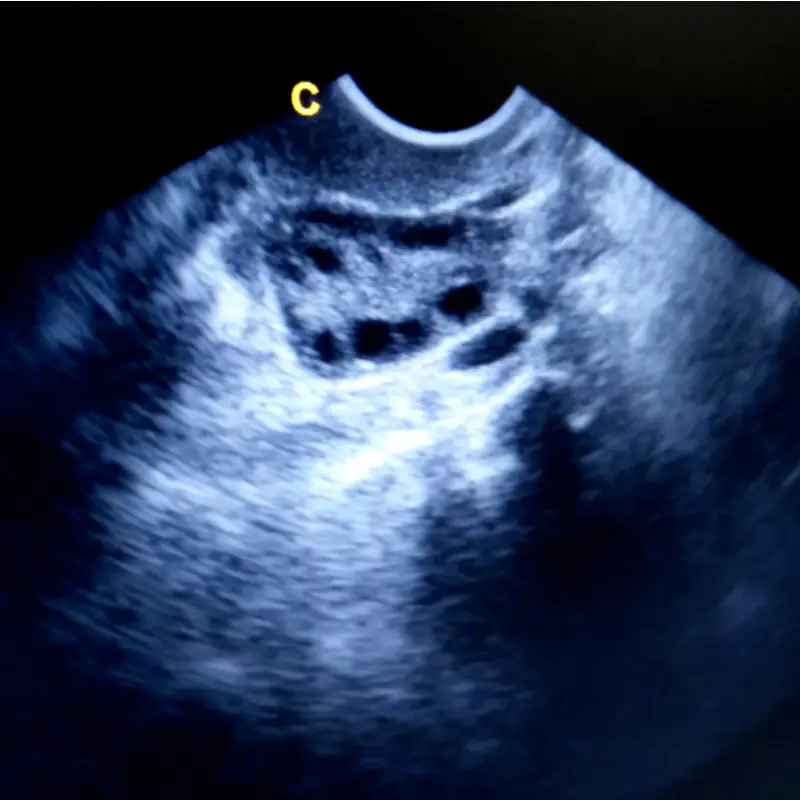
The “cysts” that are described in PCOS refer to the unique distribution (around the periphery of the ovary like a string of pearls) and higher number of follicles (measuring 2-9 mm) seen on ultrasound which is often associated with a larger ovarian volume as well.
As you can see, this is not the same thing as a persistent or recurring ovarian “cyst” which typically describes a single, larger fluid-filled follicle. No wonder why this is such a common misnomer!
Ovulatory dysfunction
When it comes to ovulatory dysfunction (either irregular ovulation or absence of ovulation altogether) this often results in irregular cycles occurring < 21 days or > 35 days apart or having < 8 menstrual cycles per year. Please note that regular cycles at irregular intervals are not normal. For example, having “regular” cycles every 45 or 60 days… not normal.
Bottom line:
The clinical presentation of PCOS varies widely and can look like many different things, making the diagnosis difficult to establish in some cases for both providers and patients.
Additional laboratory evaluation for diagnosis often involves ruling out other clinical diagnoses that can mimic PCOS like symptoms, but would be treated completely differently!
What Causes PCOS To Happen
Diagnosing a condition is only the first step towards healing the body. It’s equally important to understand the root cause of PCOS in the first place.
Why?
Because it’s not just about regulating your menstrual cycle or achieving pregnancy… It’s also about minimizing the long term health risks associated with this syndrome.
As you just learned, one of the major problems with PCOS is hyperandrogenism. Although there is still much we don’t know for sure, it’s believed that the increase in androgens is kicked off by chronically elevated levels of luteinizing hormone (LH) and insulin via multiple mechanisms.
-
Both elevated LH and insulin levels in the body stimulate androgen production by your ovaries.
-
Elevated levels of insulin also increase androgen production by your adrenal glands.
-
To make matters worse, excess insulin also suppresses the production of sex hormone-binding globulin in the liver, which in directly results in increased levels of free testosterone… which is what causes the more bothersome symptoms of acne, excessive hair growth and the like.
Another issue with excess insulin within the body is its ability to increase adiposity (i.e., body fat). And the more body fat we carry, the more insulin resistant we become. Although not all women with PCOS will have overweight or obesity, you can see how this turns into a troublesome cycle that feeds into itself.
Of course, all of the above also contributes to the irregular menstrual cycles and ovulatory dysfunction resulting from impaired hormonal signaling from the brain. Unfortunately, for many women, it’s the impact on fertility that first brings PCOS to their or their doctor’s attention.
Comorbidities Associated With PCOS
Beyond making the correct diagnosis of PCOS, and achieving pregnancy it’s important that both women and their health providers recognize that there are many comorbidities associated with PCOS that need to be recognized and addressed.
Beyond an increased risk of ovulatory infertility, women with PCOS have been shown to have a significantly higher likelihood of:
-
Impaired glucose tolerance and/or type 2 diabetes – 3-5x higher prevalence
-
Increased body mass index (BMI) – 50-80% of women with PCOS struggle with obesity
-
-
Endometrial hyperplasia or endometrial cancer – 2-6 fold increased risk
-
Depression (moderate or severe forms) – 3-4x higher odds
-
Eating disorder – 4-5x higher odds
A survey of OB/GYN providers published in Fertility and Sterility in 2017, showed that while the majority of providers (> 85%) recognized the cardiometabolic comorbidities associated with PCOS, only around half were aware of the psychological comorbidities including anxiety, depression, and reduced quality of life.
This means that as healthcare providers continue to broaden their awareness, you must advocate for yourself and seek out support because the emotional struggles you feel are real.
If you are struggling with anxiety or depression around PCOS, please know that you are not alone and there are many resources available to support you as you learn to triumph over PCOS which we’ll be covering in the coming posts.
Taking The First Steps To Beat PCOS
As you’ve probably gathered by now, PCOS is a complex disorder that can be challenging to diagnose… but successfully managing PCOS is possible if you follow proven steps.
Unfortunately, all too often, women struggling with PCOS only receive band aid treatments that fail to address the root cause.
But that’s not going to be you!
When setting out to beat PCOS, you must first be ready to make some changes to your lifestyle. And before you sigh, we know you can do this because Metformin is NOT the only answer!
More importantly, lifestyle changes that address the root cause of PCOS have additive benefits that far exceed any medication you can take (and without all those unpleasant side effects).
For the science nerds among us, there are numerous high-quality research studies that tell us which lifestyle strategies are best. And if you decide to search for the answers on the internet, maintain a healthy degree of skepticism – because there are countless claims out there with little to no scientific evidence to back them up (you know the ones we’re talking about – juice cleanses, grapefruit diets, and carbohydrate restricting).
Either way, there’s no need to fret, we cover all the lifestyle changes that truly matter in our PCOS mini-series. For now, here are the 3 most important considerations we always ask ourselves when evaluating recommendations for PCOS:
-
Consideration #1: Does it improve clinical outcomes? (Reduced hyperandrogenic symptoms, improved menstrual cyclicity, improved ovulation or pregnancy rates, etc.)
-
Consideration #2: Does it result in improved quality of life? (Reduced anxiety/depression scores, etc.)
-
Consideration #3: Is it sustainable? (Are women able to maintain it? Or are they so miserable doing it, once they stop their symptoms are worse than before or they gain even more weight than they lost?)
If all these three boxes aren’t checked, then in our book, it’s simply not good enough.
So no matter what you’re considering – diet, exercise, or supplements – stop and review these 3 considerations for yourself. We promise to break it all down for you, but our ultimate goal is to empower you to take informed action for yourself (even if we’re not around).
Final Thoughts
Understanding your diagnosis of PCOS is extremely important if you want to take control of this condition.
Remember PCOS looks different for every woman, and you don’t actually need to have cysts on your ovaries to meet the criteria for diagnosis.
After you’ve reached the correct diagnosis, make sure that you and your healthcare provider take a holistic approach when treating PCOS as there are many potential health risks associated with this condition.
And above all, be your own advocate and carefully consider which lifestyle changes will work best for you.
If you enjoyed this post, get more like it
Always evidence-based. Always actionable.
And just like a good doctor’s visit, your privacy is protected
Don't worry, you can always unsubscribe with just one click.Welcome to the tribe!
You’ve joined the OvulifeMD community. Don’t forget to check your inbox for a special welcome email.
Featured Content

Leave a comment
If you have any questions, we will be happy to answer them.
Thanks for sharing what's on your mind!
Check the thread for more insight and support.






Hello!Thank you for sharing valuable information. I hope you will share some more information about infertility treatment. please keep sharing! we are very grateful to you.