
As you’ve probably read about already, eating the right foods can boost your fertility. But…
Following any sort of diet program is tough, especially if you’re facing infertility.
Enter intermittent fasting.
This popular eating practice has received a lot of attention as an easy alternative to traditional dieting and calorie counting.
However, it raises some important considerations when you’re trying to conceive (and with pregnancy for that matter).
Here’s a quick overview of what you’ll discover:
What is Intermittent Fasting?
Despite its many forms, intermittent fasting is a dietary pattern that simply cycles between periods of fasting and eating.
Pretty simple, right?
It’s actually something most of us do every night…
(Assuming you resist those midnight snacks).
Either way, it takes about a 12 hour period of time for our bodies to use up their glucose stores before we enter a “fasting state.”
With this in mind, there are many different ways we can reduce our caloric intake when attempting to fasting.
A few of the more popular methods include:
-
The 16/8 Fast: one of the most popular forms of time-restricted eating (TRE) that involves fasting for 16 hours and then eating during the remaining 8-hour window.
-
The Warrior Diet: drawing on inspiration from ancient warrior cultures where it was believed that all meals during the day were eaten in the evening during a 4-hour period.
-
Alternate Day Fasting: a low-calorie form of fast that involves eating ~ 500-600 calories per day on alternate days of the week.
-
The 5/2 Plan: another form for fast mimicking that targets calorie restriction (~ 500-600 calories per day) to just 2 days per week with normal calorie intake the remaining days.
Bottom line:
No matter what form it takes, intermittent fasting is all about shrinking the eating window and expanding the fasting window.
What Are the Health Benefits of Intermittent Fasting?
Before we take a closer look at intermittent fasting and fertility… let’s look at why this form of dieting has received so much attention.
Thanks to bestselling books such as The Diabetes Code by Dr. Jason Fung and documentaries like Eat Fast, Live Longer, intermittent fasting has become one of the world’s most talked-about health and wellness trends.
In fact, the New England Journal of Medicine (NEJM), arguably one of the most prestigious medical journals, recently published a review article promoting the benefits of intermittent fasting.
Here’s a short excerpt from the article:
“Repeated exposure to fasting periods results in lasting adaptive responses that confer resistance to subsequent challenges….
… that leads to increased expression of antioxidant defenses, DNA repair, protein quality control, mitochondrial biogenesis and autophagy, and down-regulation of inflammation.”
And the really exciting part?
The review article makes the case that intermittent fasting can improve many chronic health disorders, including obesity, diabetes, cardiovascular disease, cancers, and neurodegenerative brain diseases.
Okay, great! But…
How does it affect fertility?
We’re about to get there, promise 🙂
In the meantime, let’s quickly look at the impact of intermittent fasting on your body weight and metabolism, as this may affect your efforts to conceive.
Intermittent Fasting & Weight Loss
When your body enters a fasting state, many metabolic changes begin to occur that support weight loss, including a shift in important hormones that regulate appetite (e.g., leptin and adiponectin).
More importantly, intermittent fasting can lower insulin levels, thereby improving insulin sensitivity and reducing insulin resistance. Women with polycystic ovary syndrome (PCOS) understand just how important this can be for a normal menstrual cycle and ovulation.
An increase in growth hormone, as well as the fat-burning hormone norepinephrine, has also been noted with intermittent fasting. As a result of these hormone changes, short-term fasting may increase your metabolic rate, further promoting weight loss.
Finally, intermittent fasting may result in less muscle loss than a more standard approach of continuous calorie restriction.
All these changes could prove highly beneficial for patients needing to lose weight before pregnancy or undergoing fertility treatments (e.g., IVF or IUI).
And this brings us to the main point of our discussion…
Is There Evidence to Support Fasting When TTC?
Spoiler alert…
There’s not a ton of great research out there on humans when it comes to answering questions about intermittent fasting’s potential impact on fertility.
Most of the information available has been done on men, post-menopausal women, and rodents. Not all that helpful, right?
Regardless, conception involves a delicate balance of hormones that can provide us with potential clues as to whether intermittent fasting is advisable when trying to conceive.
The whole process actually starts in the brain 🧠
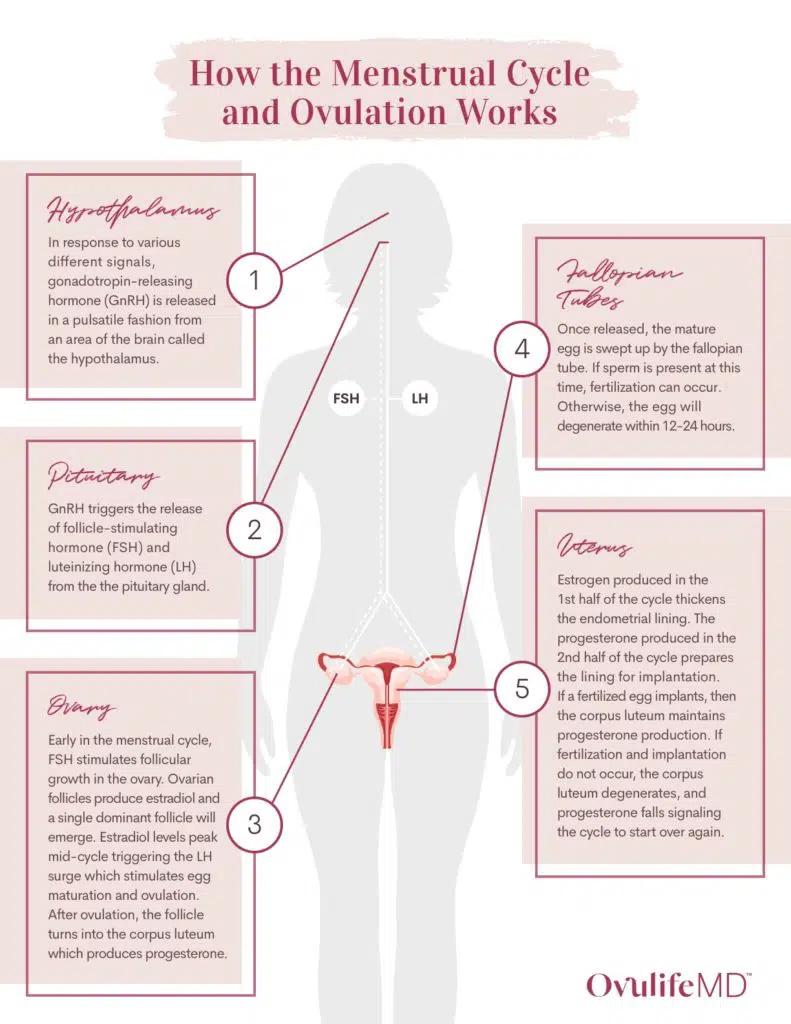
A signaling protein (that’s extremely sensitive to physical and mental stress) called kisspeptin – one of many regulatory proteins actually – is responsible for activating gonadotropin-releasing hormone (GnRH). In turn, GnRH stimulates the release of follicle-stimulating hormone (FSH) and luteinizing hormone (LH) from an area in the brain called the pituitary gland.
As you may know, in the first half of the menstrual cycle, FSH stimulates the growth of follicles in the ovaries, which produce estradiol (i.e., estrogen). Once the estradiol gets high enough, a second signal, LH, is kicked out from the pituitary which triggers ovulation from the dominant follicle which then secretes progesterone.
Okay, endocrinology lesson over!
Now here’s why this seems to matter…
The female pituitary gland is sensitive to caloric intake. Below a certain level, signaling proteins like kisspeptin could decrease, thereby causing levels of LH and FSH to drop. Unfortunately, the only studies confirming this have been done on animals.
Conversely, one study in women of reproductive-age women actually found no correlation between fasting and LH, FSH, estradiol, or progesterone. However, the intervention involved a continuous 72-hour fast and not an intermittent fasting protocol. Interestingly, this fasting protocol elevated cortisol levels and advanced secretion of evening melatonin.
As with everything in science, there’s always a caveat, and polycystic ovary syndrome (PCOS) may seem to be this caveat. It is hypothesized that intermittent fasting may improve fertility in women with PCOS by reducing levels of both insulin and glucose.
In fact, one study (which included only 15 women with PCOS) concluded that short-term calorie restriction actually increased LH levels but decreased glucose, insulin, leptin, and testosterone.
Bottom line:
Most of what we know about intermittent fasting and fertility is based primarily on how the hormones of our hypothalamus, pituitary, and ovaries should theoretically function under periods of stress.
Of course, there are many different forms of intermittent fasting, so it’s difficult to know how this form of calorie restriction truly affects our reproductive systems until more studies have been conducted and reviewed.
How to Safely Get Started
If you decide to give intermittent fasting a try, make sure to do it safe, smart, and strategically.
We always recommend discussing your decision to try this with your healthcare provider, but here are some of our top tips to get you started.
-
Start with just 1 or 2 days per week.
-
Try smaller fasting widows (e.g., 16/8 fast) in the beginning.
-
Listen to your body & stop if your menstrual cycle becomes irregular.
-
Eat pro-fertility, nutrient-dense foods when you’re not fasting.
-
Skip high-intensity exercise on fasting days.
-
Stay well hydrated and avoid excess caffeine.
-
Track your progress and energy levels.
Above all else, make intermittent fasting work for you!
If you’re overwhelmed and burnt out on your fertility journey, then your energy and attention may be best applied elsewhere. Consider the practice of mindful eating or work towards increasing your intake of fertility-boosting foods instead.
What are the possible side effects?
There are a number of potential side effects of intermittent fasting.
Here are a few to watch out for and what you can do should you encounter them:
-

Hunger. Not really an actual side effect per se, but a common issue when fasting. Intermittent fasting experts claim that this can be eased by following a keto or low-carb/high-fat diet; however, as discussed on a separate blog, going keto is not always ideal when TTC.
-

Headaches. A common occurrence during the first few fasting periods. Drinking electrolyte-enriched water or slightly increasing your salt intake may help.
-

Constipation. This typically happens with more prolonged fasting periods – it can be a normal response to eating less. Try using a stool softener to stay regular. Any significant bloating or abdominal discomfort should be an indication to stop and contact your doctor.
-

Elevated blood sugars. The hormonal changes that occur during fasting can cause your body to increase its blood sugar to provide energy. This is known as the dawn phenomenon and is not overly concerning unless your blood sugars stay elevated.
-

Irregular menses. Intermittent fast can increase the risk for irregular menses, especially in those with high activity levels or low body fat percentage.
This is not an exhaustive list of all the potential side effects, so make sure to report any new or unusual symptoms to your doctor if you choose to give intermittent fasting a try.
Looking to Optimize Your Diet and Increase Your Chances of Success?
Join Us for Our FREE Training!
Is it safe to do while pregnant?
Always speak with your healthcare provider before making any significant changes to your diet and exercise habits when you get pregnant.
With that said…
Intermittent fasting is generally NOT recommended for women during pregnancy.
This is partially due to the fact that there’s little (if any) research when it comes to intermittent fasting during pregnancy. And even though there have been a few studies looking at women who have fasted during Ramadan, they all suggested that additional research is required to evaluate potential adverse effects and other health implications that may not appear until later in life.
Ultimately, it’s important to keep in mind that pregnancy is a time to focus on:
-
Providing adequate nutrition for proper fetal development
-
Helping your baby gain an appropriate amount of weight
-
Accumulating adequate maternal fat stores for breastfeeding
And it’s for these reasons that the American College of Obstetricians and Gynecologists (ACOG) recommends that you work with your healthcare provider to develop an individual plan for weight gain (or weight loss) based on your body mass index (BMI) and overall health.
When should you avoid intermittent fasting altogether?
There are certain groups of women who definitely shouldn’t fast.
This includes anyone who:
-
Is underweight
-
Is pregnant or breastfeeding
-
Has a history of disordered eating
-
Is under a great deal of chronic stress
-
Has major medical issues, like diabetes
What Diet is Best for Fertility?
One of the most important things to remember about intermittent fasting is that it’s simply a pattern of eating – it’s not a true diet per se. This means you still need to focus on consuming high-quality foods when it comes to time to eat!
As we’ve discussed before, this involves increasing your intake of plant-based proteins, anti-inflammatory fats, and slow-digesting carbs. Of course, there’s a bit more to it, but these simple steps will keep you moving in the right direction.
For more detailed information, make sure to read our blog post on Decoding The Fertility Diet!
Final Thoughts
Intermittent fasting is an exciting topic with the potential to improve our health and wellness. However, when it comes to fertility, there’s still much to learn, especially with all the different forms of intermittent fasting out there.
There may be some circumstances in which intermittent fasting could prove to be beneficial, such as women with PCOS. It might also be an effective approach to lose or maintain weight prior to pregnancy, but it’s unlikely to be the best way to get there when you’re trying hard to conceive.
Finally, at the risk of sounding like a broken record, remember it’s a good idea to talk to your doctor or a registered dietician about any form of fasting before diving in.
Whenever you’re ready… join other women trying to conceive and enhance your diet for optimal fertility today.
If you enjoyed this post, get more like it
Always evidence-based. Always actionable.
And just like a good doctor’s visit, your privacy is protected
Don't worry, you can always unsubscribe with just one click.Welcome to the tribe!
You’ve joined the OvulifeMD community. Don’t forget to check your inbox for a special welcome email.
Featured Content

Leave a comment
If you have any questions, we will be happy to answer them.
Thanks for sharing what's on your mind!
Check the thread for more insight and support.



Dear Ovulifemd,
I just wanted to reach out and express my sincere gratitude for the valuable content you have been creating on women’s health. Your articles and resources have been invaluable sources of information and support for me and many other women.
Your knowledge and expertise on the subject are evident in the well-researched and insightful articles you write. Not only do they provide important information, but they also offer a sense of empowerment and support to your readers.
Your dedication to raising awareness and empowering women to prioritize their health is truly admirable. Your work is making a positive impact on so many lives, and for that, I am extremely grateful.
Sincerely,
Dhruv