
Ever thought about freezing your eggs?
Ever wondered what the process looks like?
What are the risks?
And how much is it going to cost?
If you’re looking for answers then you’re in the right place…
Here’s a quick overview of what you’ll discover:
What is Egg Freezing?
Egg freezing is the process through which a woman undergoes ovarian stimulation followed by the subsequent retrieval of her eggs (i.e., “harvesting”) that are then frozen for a future pregnancy.
Historically, this reproductive technology was somewhat challenging because eggs have a super high water content… This means that when labs tried to freeze them by a method known as “slow freeze,” a lot of ice crystals would form which would damage the egg.
Luckily, the process has become more mainstream over the past decade – even for those not struggling with infertility – as the technology has greatly improved making it a much more successful endeavor.
In fact, newer technology has emerged where eggs can be vitrified. The vitrification process involves a “rapid freeze” using liquid nitrogen which addresses the issue of ice crystals. As a result, the vast majority of the eggs (~95% depending on the lab) are usable at a later date.
Pretty cool, huh?
The use of this amazing technology has only continued to increase. In 2014, there were around 6000 oocyte cryopreservation cycles annually for fertility preservation compared to over 16,000 freezing cycles in 2019 according to sart.org.
Interestingly, only about 10% of women have actually returned to using their eggs 2 years after they froze them (1). But, most of the data we have on this is based on prediction models of women with similar characteristics who have undergone in-vitro fertilization (IVF) for other reasons. More on that below…
For now, let’s talk about the process of freezing your eggs.
The Egg Freezing Process
The egg freezing process starts by meeting with and discussing your reproductive goals and medical history with your fertility doctor.
A basic evaluation includes getting blood tests to establish baseline measurements of ovarian reserve such as antimullerian hormone (AMH) levels. An ultrasound to assess antral follicle count (the number of resting follicles or potential eggs in the ovary) will also occur before the egg freezing work beings.
It’s important to understand these tests don’t predict fertility or reproductive health. Instead, they give you an overall idea of the number of eggs remaining and assist with choosing a medication protocol for your ovarian stimulation regimen.
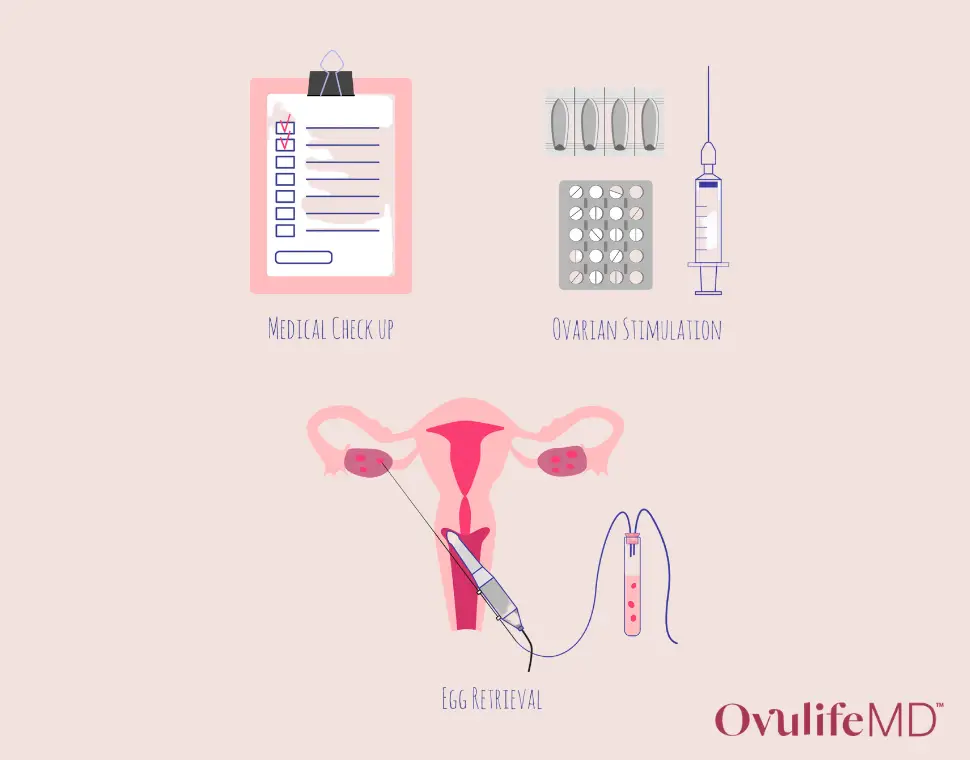
Ovarian Stimulation
If you decide to move forward, your fertility clinic may have you start oral contraceptive pills for 2-3 weeks to suppress your endogenous hormones. Some will start with your natural menstrual cycle as well.
From there, you’ll go in for a baseline ultrasound to make sure your ovaries are quiet and there aren’t any follicles or cysts that would impair your responsiveness to the injectable medications.
If everything looks good then you will start subcutaneous injections daily for a total of 9 – 14 days on average. These injections are self-administered in your stomach with a very small needle. Some come in pre-filled syringes, and some you have to mix and reconstitute yourself.
You can think of it like you’re basically giving yourself back the same hormones that your body naturally produces in a menstrual cycle (FSH and LH) at MUCH higher doses than you would produce yourself. The goal is to recruit multiple follicles and eggs as opposed to just one that’s typically released during a normal, unmedicated menstrual cycle.
Your doctor will monitor your response to the medications with a combination of transvaginal ultrasounds and blood estrogen levels. This typically requires anywhere from 4 – 7 visits over the 9-14 days of ovarian stimulation, but this can vary depending on the ovarian response. As the follicles get bigger, estrogen increases.
When the follicles are big enough, you give yourself one final “trigger” shot that causes the eggs to mature. The egg retrieval procedure will be scheduled for ~34 – 36 hours later.
Egg Retrieval
The egg retrieval itself is considered a minimally invasive procedure. It’s typically done under moderate sedation, which means you’re asleep, but you don’t need a breathing tube, so you’re breathing on your own.
Some fertility clinics do retrievals with conscious sedation (where you’re awake) and local anesthesia as well. We recommend asking the clinic you’re considering going to what their protocol is so you know what to expect from the get-go.
No incisions are required with egg retrieval and the vast majority are done transvaginally. A transvaginal ultrasound is used with a needle guide wherein the needle is inserted through the vagina and into the ovary. Occasionally a transabdominal retrieval is performed if the ovaries can’t be accessed transvaginally – the same process happens, just through the abdomen as opposed to the vagina.
All visible follicles are punctured and aspirated on each ovary and the follicular fluid (including the egg inside) is passed off to the embryologist.
The procedure itself varies in length based on how many follicles there are but is typically anywhere from 10 – 30 minutes in length.
Post-Procedure
Common symptoms post retrieval include cramping, bloating, and constipation.
It’s important to stay well hydrated after the procedure and to use a stool softener as needed for constipation or even in advance to prevent it. Cramping is typically well controlled by simple over-the-counter medications like acetaminophen (Tylenol) or ibuprofen (Motrin).
Women may continue to experience some discomfort as their ovaries shrink down after the procedure but typically they feel back to normal by their next period which is about 10 – 12 days after the procedure.
Complications are rare but possible with this procedure including bleeding, infection, or ovarian torsion (where the ovary twists on itself). All of these necessitate immediate medical evaluation.
Freezing & Banking
Once the eggs are extracted, the embryologists will strip the cumulus cells off of them (the fluffy cells surrounding the egg) to determine which eggs are mature (meaning they’ve completed their cell cycle). You may hear your clinic refer to these as “MII’s”.
Of all the woman’s eggs that are retrieved, on average ~85% of them will be mature. These eggs are then vitrified and flash-frozen in liquid nitrogen and will stay frozen until you decide to come back and use them.
More on that process below…
Health Risks and Side Effects
In addition to the procedure-related risks mentioned above, one of the biggest risks of egg freezing is ovarian hyperstimulation syndrome (OHSS).
Symptoms of OHSS can include abdominal pain, bloating, nausea, vomiting, increased fluid in the abdominal cavity, and decreased urine output. Some of the more severe symptoms of OHSS include decreased kidney function, difficulty breathing, and increased risk of blood clots. Severe cases are rare and largely preventable by avoidance of HCG for the trigger shot (using a medication called Lupron instead or a combination of both).
Ovarian torsion (where the ovary flips on itself) is also a rare but potential complication. In general modified physical activity is encouraged once women start stimulation medications and until their ovaries shrink back down to size (about 1 week after retrieval) to minimize this risk.
One last thing that to mention… At this time, the evidence does not support a relationship between the risk of fertility medications and breast or ovarian cancer (2). With that said, if you have a family history of these conditions, it’s important to discuss them with your healthcare provider.
When Should You Consider Freezing Your Eggs?
This is a GREAT question with a not so straightforward answer…
It’s incredibly important to recognize that you are born with all the eggs they’ll ever have and that egg supply decreases over time. On average, women start with about 2 million eggs at birth. By your first menstrual cycle or menarche, that total drops to about 400,000, and at age 40 most women have about 25,000 eggs left.
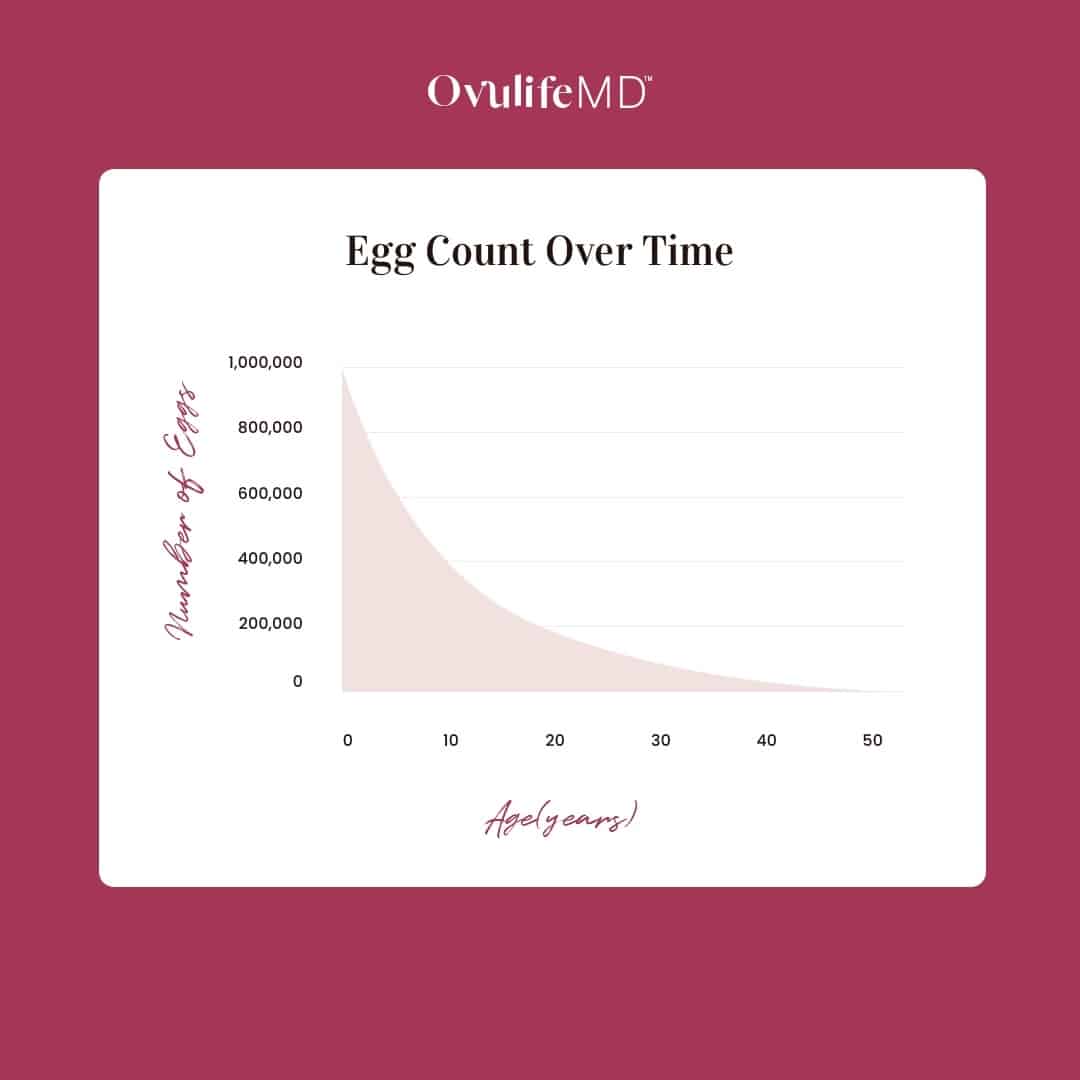
You can think about your fertility in two ways:
-

The overall number of eggs remaining (egg quantity)
-

The genetic content of those eggs (egg quality)
Ultimately, as a woman ages, both the quantity and quality of her eggs decline. So when it comes to having a successful pregnancy (and live birth) from frozen eggs, two factors are important to keep in mind: the number of mature eggs frozen AND the age when they were frozen.
Before we leaving this topic, it’s important to highlight the importance of egg quality. By the time we turn 30, there’s approximately a 23% aneuploid rate (embryos with an abnormal number of chromosomes that won’t result in a viable pregnancy). This percentage increases between 30 – 40% at the age of 35 and then to 50 – 60% at the age of 40.
Of course, your future success isn’t the only thing to keep in mind…
It’s also important to consider the likelihood that you’ll actually use them. For example, a 25-year-old who is thinking about starting her family at the age of 30 wouldn’t be nearly as likely to use her frozen eggs as a 35-year-old who is thinking about starting her family at the age of 40.
Finally, if you’ve had a recent cancer diagnosis and you are facing cancer-related treatments (i.e., chemotherapy, radiation, surgery, etc.) that may directly impact your reproductive health and ovarian reserve. Make sure to request a fertility preservation consultation ASAP to discuss your options… because you do have options!
Success Rates and Your Future Fertility
As the average age of reproduction continues to increase, fertility continues to decline. And while over 16,000 cycles were completed in 2019 alone for the purposes of egg freezing for fertility preservation, not as many women have come back to use their eggs at this point. As a result, the majority of data on future success rates with egg freezing is based on prediction models (3).
As we mentioned above, future success with frozen eggs is largely a product of 2 things:
-

The age of the woman when her eggs were frozen
-

How many mature eggs are frozen
A group from Brigham and Women’s developed a handy egg freezing calculator that you can play around with to get an idea of the impact of age and egg number on future success.
For example, a 35-year-old who has 10 eggs frozen is predicted to have a nearly 70% chance of at least one live birth from those eggs in the future. Whereas those same 10 eggs for a 40-year-old woman would yield only a 30% chance of at least one live birth in the future.
Now, this isn’t to say that women in their early 40’s shouldn’t consider freezing their eggs… it’s just important to know that it may take more than one cycle (or maybe even two) to reach your goal.
Another study looking specifically at women who actually froze their eggs and came back to use them noted the highest success in women who were 36 years of age or less, and suggested at least having 8 – 10 eggs frozen for a reasonable chance of future success (1).
It’s important to understand that nothing ever guarantees a 100% chance of success, but egg freezing would definitely offer the highest chance of protecting your ability to have a biological child in the future.
What Happens When You’re Ready to Use Your Eggs?
First off, it’s important to point out that freezing your eggs and undergoing one (or more) egg retrievals will NOT decrease your future fertility.
If you’re <35 years of age and have been trying to conceive for 12 months or more or ≥ 35 years of age and have been trying for 6 months without success… it’s probably time to revisit your fertility specialist and talk about using those eggs. Or perhaps you’ve decided to move forward as a single mom by choice. Whatever the case, don’t be afraid to use them!
Once you’re ready to use your eggs, your uterus will first be prepared for embryo implantation. This can occur with a combination of estrogen pills and patches with progesterone OR timed off your natural menstrual cycle. Ultimately the eggs will be thawed to time the development of the embryo with your endometrial lining development.
Once the eggs are thawed they are inseminated via intracytoplasmic sperm injection (ICSI) where the sperm is injected directly into the egg. On average ~85-95% of eggs will survive the thaw (ask your clinic specifically what their thaw survival rates are for your age).
Of the eggs that thaw appropriately, assuming normal sperm parameters, about ⅔ will fertilize normally and turn into an embryo. Of those, about half will grow out into a blastocyst (day 5 or 6 embryo) that can then be transferred to your uterus, biopsied for genetic testing, or frozen for later use.
It’s important to point out that the blastocyst stage is when the embryo can be biopsy for aneuploidy screening (genetic testing of the embryo’s chromosomes for abnormalities). Keep in mind, this isn’t possible with just the egg.
How Much Does Oocyte Preservation Cost?
Egg freezing costs on average anywhere from $10,000-20,000 per cycle including doctor’s visits, the procedure, medications, and storage depending on the fertility clinic you visit.
The thawing of the eggs and transfer of a subsequent embryo will be factored in separately, so it’s important to consider and ask about these financial costs as well.
Thankfully, more and more companies are following the standard set by large tech companies like Google and Facebook and are starting to cover egg freezing and fertility preservation services in their insurance plans, but we have a long way to go.
Diet and Lifestyle to Optimize Success
Now that you’ve invested all this time and effort learning about fertility preservation, what can you do to OPTIMIZE your chances of success?
Unfortunately, no studies have looked directly at lifestyle factors and outcomes in women who are freezing their eggs. But, there is excellent evidence from both the Nurse’s Health Study as well as the EARTH Study that would suggest improved outcomes in terms of egg health by consuming a pro-fertility or fertility diet.

In the months leading up to treatment, making some simple changes like eating more whole grains, incorporating more of the good fats (omega-3s) found in salmon, chia seeds, and hemp seeds, consuming more plant-based proteins in place of conventional animal meat, and avoiding deep-fried foods and pre-packaged baked goods that are rich in trans fats can all help optimize your outcome.
In terms of beverages, remove those sugar-sweetened beverages (like soda, sweet tea, or energy drinks) and eliminate alcohol intake while you’re actually taking your injectable medications. If you want a deeper dive into the Fertility Diet, search through some of our prior blog posts on the topic.
In addition to adjusting your diet, stay active while taking your injectable meds, but clear your workout regimen with your fertility doctor as some things might be a little too high intensity as your ovaries get bigger.
Take a prenatal vitamin with at least 1000 mcg of folic acid in it even though you’re not actively trying to conceive. In terms of other supplements, things like Co-Q10, DHEA, vitamin D, or vitamin E amongst others may be recommended. Ask your doctor what might be helpful for you, as every individual is different.
Final Thoughts on Fertility Preservation
Egg freezing is an amazing technology that gives women more reproductive choices.
As the average age of reproduction continues to increase, and more women delay childbearing to focus on their education and careers, there needs to be increased awareness around this important topic.
If you’ve been thinking about freezing your eggs but haven’t wanted to take the leap, start with a simple consultation to discuss your family-building goals. Get some basic blood testing to see where your egg counts are.
Start by getting the information to make an informed decision for yourself!
References
-
- Cabo A. Garcia-Velascao J, Coello A, et al. Oocyte vitrification as an efficient option for elective fertility preservation. Fertil Steril. 2016 Mar;105(3):755-764.e8.
-
Practice Committee of ASRM. Fertility drugs and cancer: a guideline. Fertil Steril. 2016 Dec;106(7):1617-1626.
-
National Summary Report. (n.d.). https://www.sartcorsonline.com/rptCSR_PublicMultYear.aspx.
If you enjoyed this post, get more like it
Always evidence-based. Always actionable.
And just like a good doctor’s visit, your privacy is protected
Don't worry, you can always unsubscribe with just one click.Welcome to the tribe!
You’ve joined the OvulifeMD community. Don’t forget to check your inbox for a special welcome email.
Featured Content






Leave a comment
If you have any questions, we will be happy to answer them.
Thanks for sharing what's on your mind!
Check the thread for more insight and support.